Project Narratives
Kenya Heart and Sole: The Afya Njema Project
June 2013 Trip
To see the pictures and narrative of June 2013 trip, visit our blog.
June 2012 Trip | June 2011 Trip | June 2010 Trip | June 2009 Trip
June 2012 Trip
The mission of the Kenya Heart and Sole: Afya Njema Project has been to address health care disparities in Kenya and provide education, screening, and treatment for non-communicable diseases such as cardiovascular and metabolic diseases. While non-communicable diseases are on the rise worldwide, preventative measures are often lacking. Through a partnership with UMass Boston, Kenyatta University School of Nursing, Tumutumu Hospital School of Nursing, and Kijabe Hospital School of Nursing, students, faculty, and clinicians are able to experience the importance of collaboration in order to address significant global health issues and begin to offer solutions for health care disparities.

|

|
| Greeting from a Kenyan colleague to the awaiting Kenyans at a community screening. | Annya provides education to a gentleman at the Kambui clinic. |
The mission started on a cold Thursday on June 19. Our team from UMass Boston headed for the villages in central Kenya. On the first days we visited schools and hospitals/health clinics in Tumutumu and Kijabe. The team also visited homes in the village of Kigumo, in order to better understand the experience of living in rural Kenya. The community immersion gave us a snapshot of how the villagers live day to day in the midst of extreme poverty. We were overwhelmed by the warmth of our reception.

|
| This is a typical kitchen in Kigumo community. The stove is made from three stones on the ground, causing the women to bend over to cook. |
While touring the various hospitals, we were all surprised by what we saw. Even the differences between the government-run Kenyatta Hospital in Nairobi and the privately-funded hospitals in Tumutumu and Kijabe were significant. The limited access to equipment that we take for granted in hospitals in the United States was startling, and made us all reconsider what constitutes quality care. We were all amazed by the level of knowledge and skill of our Kenyan partners, and even during the first few days orienting to the Kenyan lifestyle, we learned so much from each other.
The combined partners of US and Kenyan nurses were ready for their job as were the yearningly waiting communities at the screenings. The Kenya Heart and Sole team introduced the project and the purpose of the screenings, as well as described the screening layout. Each patient was registered, anthropometrics (height, weight, waist circumference, & BMI) were recorded, a medical history, blood pressure, and blood sugar were taken, education was provided, and patients were either sent home or referred back to the nurse practitioners and doctors for further evaluation. Each patient was given a copy of their results, including blood pressure, blood glucose, BMI, and waist circumference. This was significant for them because it was a tangible medical record that could be retained and presented at subsequent health care visits, providing a baseline for further monitoring. Patients were also given educational handouts on cardiovascular disease, diabetes, and nutrition, with helpful preventative strategies to reduce their risk of succumbing to a cardiometabolic disease or event.

|
|
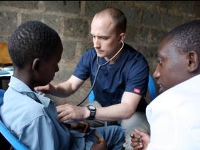
| Sofie taking a waist circumference of a Kenyan woman. | US and Kenyan nursing students collaborate to screen a young man at the community screening. |

|

|
| Jessica performing a blood glucose test. | US and Kenyan team members working together to provide education at the Kambui screening. |
The Kenya Heart and Sole trip of 2012 provided an experience of a life-time for both the US and Kenyan teams. For the students, faculty, and clinicians involved in the Kenya Heart and Sole team, this was an interaction that constructed a foundation for enhancement in their individual role in nursing and in global health. The collaboration and partnership been the US and Kenyan team has and will continue to grow stronger as we strive to perpetuate our mission.

|
| Presentation of a nursing text book from the US team to the Kenyatta University School of Nursing. |
Trip Summary:

|
| The US team members arrive in Nairobi, the beginning of an incredible journey. |
We Arrived late at night in Nairobi airport, where we met our bus driver who drove us to the Methodist Guest House (MGH).The next morning there was time to sleep in and rest to prepare for the next two weeks of hard work. We walked through a park in Nairobi to a shopping plaza where we exchanged money for shopping, and then drove to Kenyatta hospital, the largest public hospital in Kenya, with our Kenyatta nursing student partners. We saw the ICU floors, emergency rooms and general medical floors. That evening we held group discussion about what we saw that day and started preparing for the next day, organizing medications and packing our travel bags.

|
| Kenyatta National Hospital |
On the 19th, in a small very rural town Kigumo, many villagers were kind enough to show us around their homes and farms, giving gifts such as a bag of ripe avocados, or even a chicken for dinner. The generosity was overwhelming and instantly felt like we could call them a friend. We then walked to visit the primary schools, where we were able to read a few pages of a book to them. We also provided a health lesson to the young students about healthy diet choices and exercise. Later that evening, we were graciously provided dinner at Mercy's mother's house. The food was delicious and the hospitality made us feel as though we were home.

|

|
| Alain, a US team member, with a gracious Kigumo community member, showing him her home and land during a community assessment. | Children from the Kigumo primary school surrounding the bus in excitement to see the Mzungus. |

|
| Children from Thageini primary school performing traditional African dances for the US team. |
The next day, as we entered the town of Tumutumu, villagers started chasing our bus on foot in excitement and happiness to see us. On this day we visited their primary school. We were greeted with traditional African dances by the students. Again we were able to read to the children and provide a message about being heart healthy. The most rewarding part about visiting the children at both primary schools was after we took their pictures, seeing their faces light up with wonder and excitement as they saw themselves on a digital camera for the first time.

|

|
| The KHAS 2012 US team presenting children's books to the primary school. | Students from the Tumutumu School of Nursing performing a skit on cardiovascular health for the community members of Kaiyaba waiting for the screening to begin. |
We then drove to Tumutumu hospital, where we met our next nursing student partners. We listened to Margaret’s speech on pain management, and our partners gave us a tour of the surgical ward, maternity ward and their classrooms. This evening, we visited our teammate, Jacob's home in Tumutumu and were provided with a generous meal of various traditional Kenyan dishes. On the 21st, we left before the sun had risen to drive to Kaiyaba. This was our first screening of the trip. Our Tumutumu nursing student partners greeted the patients who had been waiting for us by performing a skit about primary health care. Meanwhile the undergraduate nursing students set up a large room for surveys and screenings, while the Nurse practitioners and other clinicians set up screening sites in smaller rooms.

|
| Elyse taking a blood sugar of a Kenyan woman. |
22nd- Kijabe hospital. On the drive to Kijabe Hospital, we drove passed tea farms where men and women picked tea leaves from the fields by hand, and down the mountainside overviewing the famous rift valley. After sharing a delicious lunch with our partners, we toured the hospital seeing the difference between the private and public sections, the men and women ward, the surgical building, TB and HIC clinics, and beautiful Gardens in the center of the hospital grounds.

|
| Main entrance of Kijabe Hospital. |
23rd- Screening Lari- In Lari, the screening took place in a large church where we rearranged benches and utilized the pews to set-up our equipment. The screening brought in a couple hundred people. There were many children present and when the screenings were over we learned about and participated in their popular childhood games, as we waited for transportation to arrive.

|

|
| Elyse letting a young Kenyan girl sharing a touching moment on the steps of the community screening. | US and Kenyan nursing students collaborating to screen and educate about cardiovascular disease. |
24h- Safari- Nakuru national park-As we arrived, baboons were all around the parking lot! As we drove into the park, the scenery was breathtaking. We drove through a small forest to see water buffalo, gazelle and flamingos across the plains surrounding Lake Nakuru, then up to the highest point overlooking the majority of the park. We stopped at a beautiful waterfall and cave, saw ostriches and zebras up close, and even saw giraffes chasing off a lion.

|

|
| KHAS 2012 team members enjoying a day on safari the Nakuru National Park. | Giraffe walking right next to our bus! |
25th- Screening Kigumo- The road to this medical camp was long, winding and mountainous, and the screening was set up partially outside. Before we finished our screenings, it started to downpour. We were worried we would not see everyone, but through determination and working together, we managed to screen everyone! Our bus driver Paul got us home safe along the mud roads to the MGH!

|
| Community members waiting to be seen at the Kigumo community health center. |
26th- Screening Kambui- The screening in Kambui brought in hundreds of people. We set-up in small rooms and eagerly awaited as the crowds rolled in. We even stayed until it was dark and used flashlights to see so that we could get everyone screened.

|
|
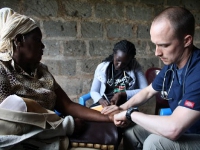
| Lines form in massive numbers at the Kambui community clinic, as the Kenyan people wait anxiously for the screening to begin. | Darren taking the heart rate of a Kenyan woman. |
27th- Elephant orphanage- On the 30th we took a day off to rest and for some us we visited the elephant orphanage. At the elephant orphanage we got up close to the baby elephants and got to read their stories of how they ended up there. Some members of the team even chose to sponsor an elephant!

|
| Baby elephant at the orphanage. |
28th- Screening Ongata Rongai- This screening was held in the urban slums of Nairobi. Most of the screening took place outside under a tent on a grassy field. It was a beautiful day and we were able screen a couple hundred people. After the screening, the members of the health clinic graciously provided us dinner at a nearby restaurant.
29th- Debriefing conference- At the MGH, we met with our team members to listen to the Ministry of Health on the future plans for supporting non-communicable disease awareness. After the conference we split into small groups to discuss our ideas as Kenyan and US nursing students about the importance of primary care and prevention, and ways to encourage awareness about non-communicable diseases. Our partners stayed overnight for a talent show, US versus the Kenyans, with dances, signing, and a group song of the National Anthem for each country. Although the Kenyans usually take home the win, US definitely gave them a run for their money this year!

|

|
| KHAS 2012 team members enjoying a night of friends with dancing, singing, and laughter. | U.S. and Kenyan team members collaborate to perform a duet. |
30th- On the last day, we said a lengthy goodbye to our partners, wishing good luck and to see each other again. Before departure to the airport, we went to the Masai Market. There was everything you could imagine from handmade wooden masks to beautiful paintings, to scarves, and handcrafted jewelry.

|

|
| At the debriefing conference, Margaret Karangatha, spoke about the impact of nursing in health care. | Guest speaker from the Ministry of health addressing plans for supporting non-communicable disease awareness in the country. |
June 2011 Trip
Many believe that the problems facing our world today can only be solved by a global, connected populace. Rather than allowing our unique positions, desires and goals to divide us, we can join our goals with those of others to both forge lasting community ties and find solutions to pressing global health issues. Nowhere is this more evident than in Kenya Heart and Sole: The Afya Njema Project.
Afya Njema's 2011 trip to the Central Provinces in Kenya brought together students from the UMass Boston CNHS and students from several Kenyan nursing schools for the purpose of providing education about and treatment of non-communicable diseases (NCD) like diabetes, hypertension, coronary artery disease, and cerebrovascular disease. The project's evolution since the inaugural trip in 2008 has coincided with the global recognition that NCDs are on the rise in Sub-Saharan Africa and present as large a health burden as that of HIV/AIDS, malaria and TB. Its goal is to improve cardiovascular health in Kenya through the development of a realistic, sustainable, culturally relevant program that emphasizes community engagement and self-management.
Students from the U.S. came from half a world away to practice nursing, to teach communities the health concerns that we in the West take for granted, and to inspire and be inspired by the experience of treating the sick in a foreign country.
Kenyan students met their counterparts to learn, gain access to specialized medicines, treat sick individuals in their communities, and develop the confidence to become healthcare leaders in their home villages and cities.
These differing motivations, brought together by the shared goals of Afya Njema Project, helped to make the 2011 trip a memorable, transformative experience for all. The following are just a few scenes demonstrating the positive social impact that occurs when people whose passions fortuitously coincide come together.

|
| The U.S. and Kenya nurses merge their strengths to serve the Mbagathi community in Nairobi |
At Mbagathi, within the city limits of Nairobi, our medical camp took place under the Acacia trees. We were fortunate to have graduate nursing students and EMTs join us alongside our now old friends, the nursing students from the University of Nairobi. Again, we were all able to work together for the benefit of the community, and reap the rewards one feels when joined in a common effort.

|
| “Mzungu” takes the BP of an elderly woman |
A “mzungu” (an affectionate term for white person) takes the blood pressure of an older woman from a rural village north of Nairobi, Kenya. Maybe it is her first time having her blood pressure taken, and it is unhealthily elevated. The nurse explains, with the help of a Kenyan nursing student from the University of Nairobi, what sorts of diet and lifestyle changes are required to bring the woman's blood pressure back to healthy levels.
Everyone leaves having learned something: the older woman how to take care of herself, the Kenyan student how to care for her community members suffering from CV disease, and the American student how to connect across cultures to help those who need it most. Everyone benefits.
The entire trip consisted of mutually beneficial interactions such as these between people whose passions coincided and collided. From the first day's tour of the Kenyatta National Hospital in Nairobi, when Kenyan students showed American students how the hospital worked, to the final day's conference with Margaret Karangatha, who helped us channel our passions into action plans and to-do lists for advancing Kenya Heart and Sole, we were all enriched by one another.
Every person touched by Afya Njema came from different backgrounds – across cultures, across disciplines and across experience levels – but all were inspired by our collaborative efforts.
Trip Summary:
The trip took place between June 11th and June 25th, 2011 in Kenya's Central Province. After a travel time of 30 hours, students met with Mercy Kamau, one of the leaders of Afya Njema, and her family. After arriving at the Methodist Guest House and resting a bit, the team toured the Kenyatta National Hospital, the largest public hospital in Kenya. Here they met the team that would be their partners and guides for the next two weeks – a group of nursing students from the University of Nairobi and their teacher, Professor Karani. The Kenyan students gave the American students a tour of the hospital.

|

|
| The U.S. team arrive in Kenya all set for a life-changing encounter. | The U.S. students are taken by their Kenya counterparts around KNH. |
The following days consisted of conducting interviews with villagers in Kigumo about the health assets of the community and setting up medical camps in four rural communities in the area to treat individuals suffering from diabetes, hypertension, and other cardiovascular diseases. At each site, we were greeted by many patiently-waiting Kenyans. Many of these men, women and children had walked for many miles just for this once-a-year treatment, check-up and education. They were as eager for treatment as we were to provide it! We were warmly received at each site by community elders, and the evenings often saw much laughter, personal connection and delicious food.

|
| A section of villagers who walked many miles for a check up & education |
This year, we had the opportunity and good fortune to stay overnight in the local centers of Kijabe and Tumutumu, and to set up medical camps to help villagers in the area. Medical students from the Kijabe School of Nursing and the P.C.E.A Tumutumu School of Nursing were our guides in these beautiful locations. When we had time off from treating villagers for NCDs, they showed us to the rim of the Great Rift Valley – the cradle of life. It was truly awe-inspiring.

|

|
| U.S. team enjoying an interactive engagement with the P.C.E.A. Tumutumu nursing students at the Tumutumu guest house. | U.S. team enjoying a breathtaking encounter with the Great Rift Valley terrains. |
We also had the chance to visit Nakuru National Park after five days of non-stop activity. We saw flamingos by the thousands, herds of antelope, giraffes and zebras scattered across the Rift Valley. Curious monkeys and baboons boldly attempted to steal our food in delightful, cheeky ways. The pure beauty of the land was breathtaking.

|

|
| A tiny section of the flamingos at Lake Nakuru in the Great Rift Valley. | Buffaloes enjoying an afternoon nap at Lake Nakuru National Park. |
Our team also set up camp at Mbagathi, which was within the Nairobi city limits. The setting differed from those of past years, but with the help of graduate nursing students and EMTs from the area, it worked. We all learned from each other how to provide quality treatment in this situation which was, in part, new for all of us. The Kenyan nursing students didn't have as much experience as we'd had with education on and treatment of cardiovascular diseases, but we didn't know the area, language, lifestyle or culture.

|
| The EMT team with the US students at Mbagathi clinic within the city of Nairobi |
One of the highlights of this year's trip was a private audience with Raila Odinga, the Kenyan Prime Minister. He listened thoughtfully to Mercy Kamau's and Eileen Stuart-Shor's presentation of the Afya Njema Project, and he readily acknowledged the critical need for our work. He expressed his hope and support for Kenya Heart and Sole, and encouraged us to expand into other villages and provinces.

|
| Eileen Stuart-Shor presents the Heart and Sole agenda and achievements to the Prime Minister (center) during a private meeting at his office. |
Our final day was spent in conference with Margaret Karangatha, the dynamic and inspirational Managing Director and CEO of the Africa Institute of Management Development (AIMD). She helped us develop a to-do list of ways to improve upon the great work we've already begun. It was clear that our programs had done much to work toward ways of rolling out non-communicable disease treatment camps and centers throughout the rest of Kenya. Specializing in organizational planning and leadership, she gave us some excellent ideas for how to grow and expand Afya Njema for next year.

|
| The Kenya and US team final day debriefing conference at Methodist guest house. |
What We've Done and Where We're Going:
This is the fourth year of Afya Njema, and it is always encouraging to see the impact of our work over the past years. We saw many returning patients, and we were pleased to see the changes they made to improve their health. Every year, we see more patients, and we expect that the project will only grow in size and scope in the years to come.
The inaugural Afya Njema trip in 2008 only consisted of three providers/researchers, screened 250 individuals, and visited three hospitals and three rural communities. This year, a team of twenty screened over one thousand people in five rural and urban locations, in addition to visiting three hospitals. We provided education and medical management of cardiovascular and metabolic disease in both Kikuyu and Kiswahili. We significantly expanded the pain management component of our program by distributing Kiswahili-language pamphlets on knee and back pain developed by Dr. Margaret Caudill-Slosberg.
|
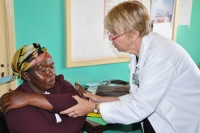
| Dr. Margaret Caudill-Slosberg assesses a client with pain. |
The work and collaboration developed on the 2011 trip will continue throughout the year at UMass Boston, the University of Nairobi, and the Kijabe and Tumutumu nursing schools. We are in our fourth year, and a long future lies ahead of us. There is still much work to be done. It will take all of us, working together in different capacities, from different cultures, toward the same goals, to fully address the problem of cardiovascular disease in Kenya and other developing countries.
The Afya Njema community continues to grow. Everyone who has had a hand in this project has given it something that it previously lacked – a new perspective, a different set of skills, or even just a level of infectious enthusiasm. We all look forward to continuing the work, sharing ideas, and strengthening our relationships with students and health professionals in Kenya. This is only the beginning of the journey to develop solutions to non-communicable diseases in developing countries. If there's one thing the Afya Njema trip has taught us, it is that these solutions can't be found alone.
UMass Boston Team Members:
Leaders
Eileen Stuart-Shor (CNHS faculty)
Mercy Kamau (doctoral student)
Margaret Caudill-Slosberg, MD (visiting faculty from Dartmouth Medical School)
Kathryn Blum ANP (CNHS faculty)
Mentors
Joelle Chatauneuf (MSN graduate)
Alia MacPherson (BSN graduate)
Georges Chick, RN (alumnus)
Megan Suyematsu (senior undergraduate)
Students
Jennifer Nugent (MSN graduate)
Monica Crowley (nurse practitioner student)
Kaitlin Brown (nursing student)
Jessica DeMita (nursing student)
Kristine Kelley (nursing student)
Kerry Parsons (nursing student)
Shannon Sayer (nursing student)
Yusil Soriano (nursing student)
Tyler Warren (nursing student)
Yevin Roh (premed student from UMass Amherst)
Andrea Sheldon (anthropology student from University of Vermont)
June 2010 Trip
A delegation of students and faculty traveled to Kenya’s Central Province to carry out our third annual Medical Mission from June 10th – 21st. The UMass Boston CNHS medical team included Eileen Stuart-Shor (faculty), Mercy Kamau (doctoral student), graduate nurse practitioner students Joelle Chateauneuf and Ijeoma Julie Eche, Kevin McDevitt (Graduate Global Health Students); returning undergraduate students Brenda Manso, Natalie King, Alia MacPherson, Erica Miranda; undergraduate students Karolina Bielecka Calamaio, Sarah Foreman, Kaitlin Allen, Megan Suyematsu, Julia Kimotho, Jillian Phelan, Georges Chick, Katie Stuart-Shor; visiting faculty Margaret Caudill-Slosberg MD (Dartmouth Medical School), CNHS alumnus Shanna Smith and Heather Milton (Exercise physiologist from Brigham and Women’s Hospital).
The mission of Kenya Heart and Sole: The Afya Njema Project is to work with our Kenyan colleagues to improve cardiovascular and metabolic health through the development of a feasible, sustainable culturally relevant CV/metabolic risk reduction program that emphasizes community engagement and self-management. We worked with our Kenyan partners to develop health solutions for larger populations, yet time and again, it was the engagement with individuals that changed our lives. Kenyans we cared for were touched by what we did, and our lives were transformed by what we saw. The Afya Njema Project may be an outreach program by UMass Boston to work in partnership with hospitals and schools in Kenya, but it was also the journey of a group of individuals who wanted to make a difference in the lives of others.
The journey began with a trip through three continents, four stops, and a late-night arrival at Nairobi Jomo Kenyatta International Airport. We were greeted with open arms by the ever-joyful Mercy Kamau and her family, all warm smiles despite the hour, and got on the matatu (bus) to get to the Methodist Guest House where we would spend the next ten days. Excitement bubbled through the group as we unpacked and prepared for the work to come.
Once we oriented ourselves and got snacks, the first order of business: we were off to Kenyatta National Hospital in Nairobi. After a warm welcome by Professor Karani and graduate students from the University of Nairobi, we toured the hospital. Kenyatta Hospital is the largest public hospital in Kenya, and is roughly twice the size of Massachusetts General Hospital. We were fortunate to have the University of Nairobi students’ guidance and perspectives on health care in Kenya as we toured the facilities. Nurses and other clinicians worked tirelessly under difficult conditions with up to 300% bed occupancy. Imagine the challenge of a daily census of 2,500 patients with 1,800 beds. We were humbled, then motivated, by the challenges that lay before us.

|

|
| Mercy Kamau at Nairobi airport welcoming the team to Kenya with open arms. | Team aboard a Matatu (Bus) with smiles from the airport to the Guest house. This Matatu was the daily mode of transport for the team. |
After touring Kenyatta we spent the night prepping and organizing all the supplies that we brought. We went over procedure and protocol for clinic the following day, eager to get to work and be of service to the community.

|

|
| Team touring Kenyatta National Hospital, Kenya’s largest government hospital. | Team organizing medical supplies and going over procedure and protocol for health screenings. |
The next morning, we took off to Kigumo, a village north of Nairobi, to do a community assessment. Kenya: Heart and Sole had done work there in previous years, and we were warmly welcomed with tea by the Village Chief Daniel Gatimbii and his family. With the help of the Chief’s family and volunteers, students went into the homes of villagers and gathered information about the community’s health assets. Students inquired about the schools, markets, water supply and health clinics, as well as about income, common health conditions, and community perception of need. This information would allow us to tailor recommendations to the village’s specific needs, and would help us understand the village environment’s influence on the health of the community.

|

|
| Dr. Caudill-Slosberg conducting a community assessment in Kigumo Village. Approaching are three village women going to the coffee factory carrying coffee beans on their backs. | Mercy Kamau’s auntie preparing ugali (corn/maize meal) for her family. Like many other families in the village they welcomed us to their home with open arms during the community assessment. |
At the day’s end, we were treated to a wonderful dinner by Mercy Kamau’s family. They honored the work of the group by inviting us to plant a tree behind their compound. Eileen Stuart-Shor did the honors, truly giving the Afya Njema Project tangible roots in Kenyan soil.

|

|
| Eileen Stuart-Shor planting a mango tree at Mama Mercy’s home. The tree was to honor the team for their work including promoting eating of fresh fruits and vegetables | Dinner for everyone at Mama Mercy’s. |
With the help of students from the Kijabe Hospital School of Nursing and the University of Nairobi, we split into two teams and set up medical camps in Kambui and Kigumo Health Centers. Word had spread about the wazungus’ (an affectionate term for white people) arrival and we were kept busy by many new patients, as well as some from previous years. To our great joy, many had taken our advice to heart and made changes to improve their health. Support from the Ministry of Medical Services this year allowed us to collaborate with the community health centers, a partnership that is critical to the success of this project. Thanks to many generous donors, we were able to provide hypertension, diabetes and pain medications to patients in need.

|

|
| Natalie King, Jillian Phelan and Sarah Foreman conducting a health screening on patients at Kigumo Health Center. | Katie Stuart-Shor taking the medical history of a patient during a health screening at Kambui Health Center. |
Of course, what would be a trip to Kenya without some views of the local wildlife? Kenya is a beautiful country and no place shows that beauty quite like Nakuru. With over 600 km of land, the animals in this national park are free to roam and a delight to watch.

|

|
| Picture of zebras mixing with the flamingos taken by the team during a safari trip at the Nakuru National Park. Going on a safari was one of the highlights of the trip. What a beauty! | Giraffes walking free through the Rift Valley; an incredible sight to see. |
After a day on safari at Nakuru National Park, where we saw herds of antelope and giraffe and thousands of flamingos mixing with zebras at the lake, we were ready and eager to get back to work.
The UMass Boston team split up, one half going to the Kijabe and the other to the Tumutumu Hospital School of Nursing. The Kijabe hosts, Principal Mary Muchendo and tutor Peris Kibiare, and the Tumutumu hosts, Deputy Principal Irene Ndigirigi and tutor Jacob Kariuku, greeted us warmly and introduced UMass Boston students to their Kenyan student partners. The Kenyan students gave us a tour of their school and hospital, and we were struck by the ease of rapport between the students. They were on the same page in no time! We didn’t think we would have much in common with students and faculty halfway around the world, but we all spoke the language of nursing, with its urgency toward caring and community service, and that shared language brought us together.
While the students toured the hospital, learning and teaching both verbally and nonverbally alongside their Kenyan partners, the faculty at each site came together to discuss chronic disease, research, and evidence-based practice from a (similarly) global perspective. The day ended with the UMass Boston faculty giving guest lectures to the school and hospital communities.

|

|
| Tumutumu Team in respective school’s uniform after a long day of lectures and touring Tumutumu Hospital. | Kijabe Team in respective school’s uniform after a long day of lectures and touring Kijabe Hospital. |
The next few days were filled with community outreach screenings in the areas and villages surrounding the hospitals. We carried out medical camps at the Lari Health Center in Kijabe and the Kaiyaba Health Center in Tumutumu. All together at the four medical camps we screened over seven hundred individuals from the Central Province around Nairobi and provided education about how to prevent and treat cardiovascular/metabolic diseases in native Kikuyu and Swahili dialects.
Thanks to PCNA (Preventive Cardiovascular Nurses Association), we were able to develop a risk stratification tool to identify those at high risk of developing cardiovascular disease. We worked in collaboration with clinical officers in the clinics to provide treatment to high-risk patients. The fact that we had medications was a tremendous asset this year, and the addition of a pain specialist to our group allowed us to provide detailed pain assessment and treatment to the communities.

|
|
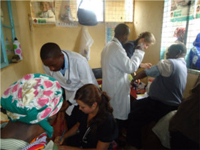
| Mercy Kamau educating people about cardiovascular/metabolic disease in the native Kikuyu and Swahili dialects. | Meagan Suyematsu and Kaitlin Allen conducting a health screening at Kaiyaba Health Center. |

|

|
| Tumutumu Team after a long tiresome day of health screening at Kaiyaba Health Center. | MeKijabe Team after a long tiresome day of health screening at Lari Health Center. |
Preliminary clinical data from the medical camps revealed a high prevalence of hypertension. More than one out of every two individuals screened (60%) had high blood pressure meaning that their systolic blood pressure was greater than 140/90 mm Hg. Fourteen percent met the criteria for glucose intolerance (diabetes) and 47% met the criteria for being overweight or obese, while 60% had two or more risk factors for developing cardiovascular disease.
Our initial community assessments showed that residents engaged in at least one hour of vigorous activity per day, had low rates of smoking, ate diets high in carbohydrates and salt with little protein or fruit, and consumed little or no soda or prepared foods. These health behaviors do not fit with our standard Western understanding of cardiovascular disease risk factors. Over the course of the year, we will have to work hard with our Kenyan colleagues to understand these findings and plan appropriate medical interventions for the June 2011 trip.

|
|
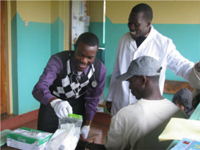
| Kevin McDevitt registering people for health screening, conducting initial assessments and giving out educational materials at Kambui Health Center. | Georges Chick checking blood sugar on a patient during screening at Lari Health Center. |

|
|
| Alia MacPherson taking patient medical history and conducting a health screening at Kaiyaba Health Center. |
We spent our final day in conference, debriefing about the week’s events and making plans for how to set up sustainable, realistic improvements in the communities. We were truly blessed by the opportunity for transnational scholarly exchange, and humbled by the wisdom and openness of everyone involved. We left with a greater appreciation of the work and knowledge our colleagues in Kenya had to contribute and with a sense of gratitude for what we had to share.
If we are ever to achieve global solutions to non-communicable diseases in developing countries, it will all depend upon locally-rooted, rich, rewarding collaborations such as those we enjoy with our Kenyan counterparts. Global health is not a matter of the place to which you travel, but the community that you carry with you on the journey, of which you are a part. Health across the globe impacts health across the globe. We cannot claim to have solved the problem of cardiovascular disease in Kenya, but we strengthened relationships, shared ideas, and kept the flow of communication moving in a positive direction.

|

|
| Mercy Kamau addressing UMass Boston, Tumutumu and Kijabe Hospital Schools of nursing and the University of Nairobi students and faculty team during the debriefing conference at the Methodist Guest House in Nairobi, Kenya. | Margaret Karangatha, the guest speaker at the debriefing conference, spoke about nursing leadership in health care. |

|
|
| Boston and Kenya team at the debriefing conference in Nairobi. |
Kenya Heart and Sole was a success on many levels. We continue to refine community and patient data obtained during the screening, and we continue to use that data to collaborate with our Kenyan partners to propose clinical and policy recommendations. The energy in both Kenya and UMass Boston for the Afya Njema Project continues to build. Students and faculty at Kijabe and Tumutumu regularly conduct cardiovascular/metabolic screenings within the surrounding Kenyan communities, and all of our partners are actively engaged in developing programs of research. At UMass Boston, students continue to communicate and collaborate with their Kenyan partners on ideas that contribute to our understanding of global health.
On this transnational journey, we learned the lesson of the power of one: “To the world you may be one person, but to one person you may be the world.” (Heather Cortez). Imagine the power of one plus one plus one ad infinitum. The Kenyans have a word for this idea: harambee (all pull together). And so, the journey of pulling together, harambee, for Kenya Heart and Sole: The Afya Njema Project begins for our next trip.
If you are interested in more information about the project please contact Eileen Stuart-Shor or Mercy Kamau.
If you would like to see more pictures, or learn more about the project check out our Facebook page.
We gratefully acknowledge the support of the following groups/grants that made this trip and the supplies we brought possible:
- Joseph P. Healey Grant
- PCNA
- Sigma Theta Tau, Theta Alpha Chapter
- Office of Global Programs, University of Massachusetts Boston
- Joan Saffron Family Foundation
- The Virginia Travers Lynch Foundation
- Endowed Faculty Career Development Award
- McNair Fellows Program
- Horizon Scholars Program
- AmeriCares
- MAP International
- Private Donations
- Team members who all paid for their own travel
June 2009 Trip
A delegation of students and faculty traveled to Kenya’s Central Province to carry out our second annual Medical Mission from June 10th – 21st . The UMass Boston CNHS team included Eileen Stuart-Shor (faculty), Mercy Kamau (doctoral student), Natasha Begon (NP student); undergraduate students Brenda Manso, Natalie King, Maddie Gamble, Lauren Robbio, Alia MacPherson, Erica Miranda, Jennifer Modliszewski, Jennifer Harrison, Yevin Roh, Lyns Hercule, Patricia Dembro, Sandy Jones; and CNHS alumnus Shanna Smith.
Although we primarily think of infections diseases when we think of Africa, non-infectious diseases, particularly cardiovascular disease and diabetes, are on the rise in the developing nations of sub-Saharan Africa. In 2007 at the Diabetes Summit in Kenya, the World Diabetes Foundation announced that “What HIV/AIDS was in the last 20 years of the 20th century; cardiovascular disease, diabetes and its consequences will be in the first 20 years of this century” (Diabetes Programme 2008). In fact, the very day we left Boston for Nairobi the National Institutes of Health (NIH) issued a press release announcing that they have established a collaborative global network of Centers of Excellence in low and middle-income countries throughout the world dedicated to furthering our understanding of the many factors involved in the development, progression and treatment of cardiovascular/metabolic disease. This was followed the next day with an editorial in The Lancet which acknowledged that the global health landscape is rapidly shifting away from one dominated by infectious diseases to one characterized by various chronic conditions, particularly cardiovascular and metabolic disease. (published online June 11, 2009). It was serendipitous that the day we left Boston for Kenya the NIH released this press report and attests to the fact that this work is timely and important. For many developing nations such as Kenya where the burden of chronic disease crisis is just becoming known, the prevention and treatment of cardiovascular disease and diabetes has implications for education, practice and policy.

|
|
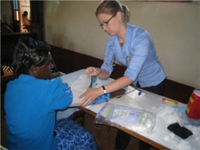
| UMass Boston NP student Natasha Begon assessing heart sounds at Kijabe Town screening location. | UMass Boston student Jennifer Modliszewski doing blood pressure screening at Tumu Tumu screening location. |
The mission of Kenya Heart and Sole: The Afya Njema Project is to improve cardiovascular health in central Kenya through the development of a feasible, sustainable culturally relevant risk reduction program that emphasizes community engagement and self-management. In partnership with Kenyan nurses and communities the project is focused on surveillance, prevention and control of cardiovascular/metabolic risk factors and diseases. Through the partnership, UMass Boston and Kenyan students and healthcare provides have the opportunity to exchange ideas about prevention and healing.
This year's trip included visits to Tumu Tumu and Kijabe Hospital Schools of Nursing, a community assessment in Kigumo and community outreach screenings in Kambui, Escarpment, Kijabe town, Tumu Tumu and Ihururu.
Our first stop was a very busy screening at the Kambui clinic. This was our second visit to this clinic and word had spread about the screening last year. Many people walked a great distance to come to the screening. Our hosts were: Kennedy Njogu (Chief Clinical Officer) and Beth (Lab technician). This year we were able to add a second day at the clinic where the NP team worked with the Chief Medical Officer to prescribe hypertension and diabetes medicine that were filled at the clinic. Our goal is to work with the Kambui clinic to carry out community-wide cardiovascular/metabolic screenings and to begin to plan for follow-up care. We are also hoping to be able to fundraise to purchase targeted medications as well as an autoclave and centrifuge for their lab.